What Is a Fan?
As we all know, ventilators are in short supply in hospitals around the world, and patients who develop respiratory distress as a result of the coronavirus may not receive the help they need to breathe.
The number of patients with COVID-19, which required aggressive assistance in breathing, is still relatively small compared to the total number of infections, but the United States and other countries are preparing to ration equipment , asking manufacturers to accelerate their production and even create improvised devices ventilator. diving masks . Some hospitals are figuring out how to use one ventilator for multiple patients.
So what is a ventilator and how sick do you have to be to need one?
Fans 101
A healthy person can breathe in oxygen and release carbon dioxide at a normal rate to keep the body functioning. But a person with sick or damaged lungs cannot breathe normal air fast enough or with enough intensity to meet their body’s oxygen needs. The ventilator does this job by creating pressure to open the lungs, delivering oxygen to the lungs through a tube, and removing carbon dioxide that the lungs create.
When you breathe, your diaphragm and other chest muscles contract, causing your chest to expand and create negative pressure to draw oxygen-rich air into your lungs. You exhale carbon dioxide when these muscles relax and your breasts return to their normal size. If your body cannot create this negative pressure on its own, you can use a ventilator to create positive pressure, pumping air instead.
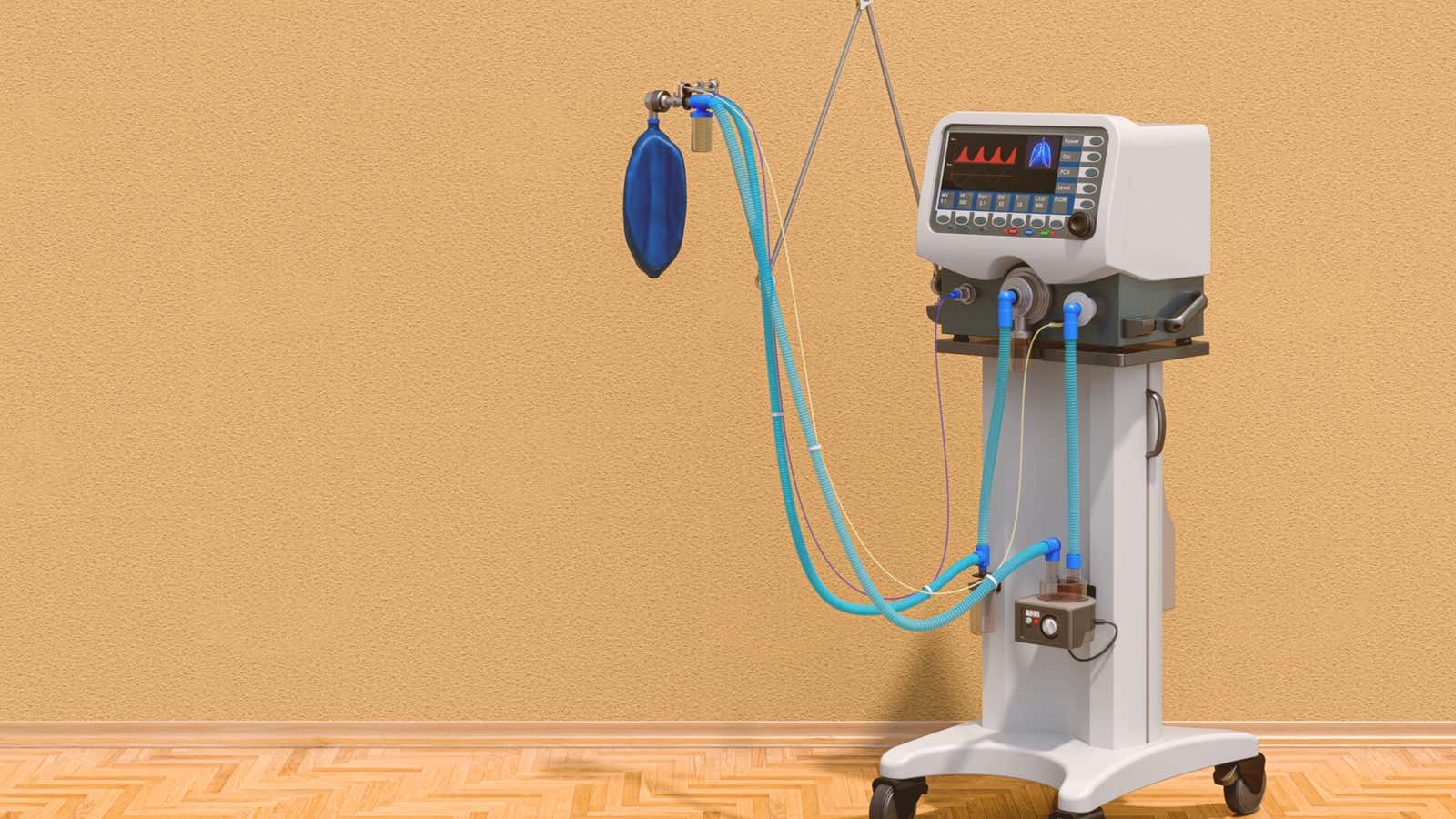
Mechanical ventilators used in intensive care facilities are large, complex devices that operate on a power source and are connected to a central oxygen source. The main body of the device is a monitor with dials, displays and settings that can be adjusted to suit the breathing needs of each patient.
Inside the case is a bellows that – like the Ambu bag that paramedics used on TV – pushes oxygenated air through a series of tubes into the lungs.
Before reaching the patient, the air passes through a humidifier, which heats and humidifies the patient. From there, oxygenated air is pushed through a tube that delivers it to the lungs and removes the resulting carbon dioxide.
Patients who are ventilated are usually intubated, which means that they have a tube inserted through their mouth into their airways. Once the endotracheal tube is in place, its end inflates, closing off the airway, which prevents gas or liquid from leaking back when air enters the lungs.
Intubated patients are also at least partially or wholly sedated on ventilators. In addition to the discomfort of having a tube pierced down your throat, it can feel like you are choking, choking, or drowning .
There are less invasive breathing aids, such as oxygen through a mask, but supplemental oxygen may not be enough for a COVID-19 patient.
COVID-19 affects the respiratory system, which is why people with pre-existing lung conditions are already half a step behind, said Dr. Brian Redmond, an anesthesiologist in Savannah, Georgia. Smokers, the elderly, and patients with other respiratory problems have less efficient lungs and may be more affected by the respiratory problems caused by the virus.
Why is there not enough fan?
When there is no global pandemic, patients are still on mechanical ventilation. But many of these people need machines for only a few hours (for example, during an operation) or for a few days, and then they are passed on to the next patient. COVID-19 patients with respiratory failure often require mechanical ventilation for a week or more, so machines do not release at the same rate.
“The reason for the bottleneck is that there are too many sick people, and when they leave, they stay for a long time,” said Redmond.
In addition, a ventilator is not a “set and forget” device. This requires constant monitoring and frequent fine-tuning to balance pressure, volume, oxygen percentage and respiration rate for each individual patient – this means that having a large number of people on ventilators requires the resources of already busy hospitals, nurses, etc. and doctors.
An additional obstacle associated with COVID-19 is that medical personnel must wear personal protective equipment – gowns, masks, gloves, glasses – every time they interact with a patient. That means they can’t just walk in and turn the dial to tune the car, Redmond said. There is also a risk of contracting the virus during intubation.
There are risks to patients who remain on ventilators for long periods of time, but Redmond says this is not a major concern for the coronavirus.
“We’re just trying to make these people survive,” he said.